Respiratory System
Respiratory System Lecture Notes–Warm Up
Airway
- General Information:
- The chief function of the respiratory system is to supply body tissues with oxygen and eliminate carbon dioxide.
- The respiratory system consists of the nasal cavities, pharynx, larynx, trachea, bronchi, and lungs.
- The nasal cavities, pharynx, larynx, trachea, and bronchi constitute the airway.
- Nose
- The nose has two nasal cavities, which open on the face through the anterior nasal apertures called the nares. The nasal septum separates the cavities.
- The anterior portion of the septum is composed of hyaline cartilage. The posterior portion is composed of bone called the vomer and the perpendicular plate of the ethmoid bone.
- Each nasal cavity has three mucosa-covered structures called the superior, middle, and inferior conchae.
- The nasal cavities are lined with hairs that trap dust and foreign particles.
- Epithelial cells lining the nasal cavities secrete mucus, which collects foreign particles which are then moved by cilia toward the pharynx, where the particles and mucus can be removed by swallowing, sneezing, or spitting.
- The paranasal sinuses, which surround and drain into the nasal cavities, are located in the frontal, sphenoid, and maxillary bones.
- Pharynx
- The pharynx is also known as the throat.
- Acts as a passageway for air and food. It also functions in speech, changing shape to allow phonation of vowel sounds.
- The entire pharynx is composed of striated muscle and lined with mucous membrane.
- The pharynx has three divisions…
- Nasopharynx
- Oropharynx
- Laryngopharynx 4. Larynx
- The larynx is called the voice box. It is a triangular organ in the front of the neck. It extends from the 4th to the 6th cervical vertebrae, attaching to the hyoid bone.
- The larynx is composed of muscle and numerous cartilages
- The true vocal cords are a pair of horizontal folds that project into the laryngeal cavity. They are separated by a space called the glottis.
- The epiglottis, which overhangs the larynx, prevents food from entering the lungs.
- Trachea
- The trachea is also called the windpipe.
- It is a membranous tube measuring 10 to 12.5 cm long.
- On entering the mediastinum, the trachea branches into the right and left main bronchi at the 5th thoracic vertebrae.
- Dorsally, the trachea contacts the esophagus.
- The trachea has a series of C-shaped cartilage rings to strengthen the trachea and prevents it from collapsing during inspiration.
- The trachea is lined with ciliated pseudostratified columnar epithelium containing mucus-secreting goblet cells, which trap and propel inhaled debris upward to the pharynx for removal through coughing.
- Bronchi
- The right and left primary bronchi branch from the trachea.
- The secondary bronchi are smaller passageways that branch from the primary bronchi. The right primary bronchi divides into three secondary bronchi and the left branches into two secondary bronchi.
- The secondary bronchi branch into tertiary bronchi which then branch into smaller bronchioles which branch into progressively smaller tubes until they branch into alveolar ducts, which terminate in clusters called alveoli.
- Alveoli are tiny air sacs lined with thin squamous epithelium. They are surrounded by capillaries where oxygen and carbon dioxide are exchanged.
- Lungs
- The lungs are paired, cone-shaped organs that fill the pleural divisions of the thoracic cavity. They extend from the root of the neck to the diaphragm.
- The right and left lungs are separated by the heart and other mediastinal structures.
- Each lung is enclosed in a pleura, a protective, double-layered serous membrane. The parietal pleura lines the wall of the thoracic cavity. The visceral pleura covers the lung directly. The space between the two membranes contains fluid, which lubricates the lungs as they expand and contract.
- Lobes
- The right lung is divided into three lobes. The left lung, smaller than the right, is divided into two lobes. It contains a concavity called the cardiac notch, which is molded to accommodate the heart.
- Blood Supply
- Blood circulates through the lungs via the pulmonary and systemic circulatory systems.
- In pulmonary circulation, the pulmonary arteries branch profusely into the pulmonary capillaries which surround the alveoli.
- In systemic circulation blood travels directly to the lung tissue. Bronchial arteries supply the lung tissue with blood.
- Breathing:
- Inspiration occurs when the diaphragm contracts, moving downward, and the intercostal muscles expand the size of the chest cavity. The increase in the size of the chest cavity reduces pressure within it and air moves from the outside high pressure to the low pressure inside the lungs.
- Expiration occurs when the diaphragm and intercostal muscles relax and therefore reduce the size of the chest cavity. This increases air pressure and air moves out. The elastic recoil of lung tissue aids in expiration.
- Lung Capacity
- Tidal volume is the normal breathing volume.
- Vital capacity is the maximum amount of air that can be moved out of the lungs after a maximum inspiration and expiration. Vital capacity volumes vary according to age, health, gender, and health.
- Total lung capacity is about 6,000 mL.
Total lung capacity = vital capacity + residual volume.
- Although tidal volume is 500mL, about 150mL of this air never reaches the alveoli. It fills the upper respiratory passages and is exhaled with the next breath.
- The upper respiratory passages contain that air is called dead space. As a result of this space, only 350mL of new air enters the alveoli with each breath and mixes with air already in the lungs. This slow replacement of air has several advantages.
- The slow mixture of atmospheric air with alveolar air prevents wide fluctuations in oxygen and carbon dioxide levels. Wide fluctuations could produce adverse effects.
- Because oxygen and carbon dioxide in the blood are in equilibrium with their gas forms in the alveolar air, stable concentrations of alveolar oxygen and carbon dioxide promote stable concentrations of these gases in arterial blood. 12. Gas Exchange
- Air exerts a total pressure of 760 mm Hg at sea level.
- Air contains about 21% oxygen. The partial pressure of oxygen is 21% of the atmospheric pressure 760 mm Hg. So the partial pressure of oxygen is 159.6 mm Hg.
- Gas concentrations in inspired air…
- Nitrogen = 79%
- Oxygen = 21%
- Water vapor = .5%
- Carbon dioxide = .04%
- Gas concentrations in alveolar air…
- Nitrogen = 74.9%
- Oxygen = 13.6%
- Water vapor = 6.2%
- Carbon dioxide = 5.3%
- Gas concentrations in expired air…
- Nitrogen = 74.9%
- Oxygen = 15.7%
- Water vapor = 6.2%
- Carbon dioxide = 3.6%13. Gas diffusion
- In diffusion substances move from an area of higher concentration to an area of lower concentration. A gas diffuses from an area with a high partial pressure of the gas to one with a lower partial pressure.
- Transport of oxygen
- Oxygen is transported by the blood in two different methods.
- About 3% of oxygen is dissolved in blood plasma
- The remaining 97% is chemically bound with hemoglobin. Oxygen uptake by hemoglobin is most efficient in the lungs where the oxygen concentration is high. Oxygen release occurs most readily in the tissues where the oxygen concentration is low.
- Lower blood pH and higher temperatures of actively metabolizing tissue, which occurs during vigorous exercise, also enhances oxygen release from hemoglobin.15. Transport of carbon dioxide
- Carbon dioxide is transported by three different methods.
- A small amount is dissolved in the blood plasma
- Some is loosely combined with amino groups in the hemoglobin molecule.
- Most of the carbon dioxide is converted in erythrocytes to bicarbonate by the enzyme carbonic anhydrase. Erythrocyte uptake of carbon dioxide begins in the capillaries.
- In the erythrocyte, the hemoglobin releases oxygen to supply the tissues. At the same time, carbon dioxide diffuses from the tissues into the erythrocytes where enzymes help turn carbon dioxide and water into carbonic acid. H2O + CO2 à H2CO3.
- Then carbonic acid dissociates into hydrogen ions (H+) and bicarbonate ions (HCO3 -). The hemoglobin molecules take up the hydrogen ions. The remaining bicarbonate ions accumulate until their concentration in the erythrocyte exceed that in the plasma, then the excess will diffuse out into the plasma.
- Simultaneously, chloride ions diffuse into the erythrocyte to replace the bicarbonate ions. Then the bicarbonate ions combine with plasma sodium and form sodium bicarbonate.
- At the lungs the whole process reverses and carbon dioxide diffuses into the alveoli and is exhaled.16. Control of Respiration
- A control center in the brain stem, called the respiratory center, regulates the rate and depth of respiration.
- This center discharges impulses to neurons that innervate the diaphragm and intercostal muscles.
- Neurons in the respiratory center are stimulated directly by increased arterial concentrations of carbon dioxide and hydrogen ions.
- During exercise, more carbon dioxide is produced. This stimulates the respiratory center to increase respiratory rate and depth.
- Chemoreceptors in the aortic arch and carotid sinus detect levels of carbon dioxide and convey impulses to the respiratory center.
- Receptors in the lungs respond to stretching as the lungs inflate, sending impulses to the respiratory center to inhibit further inspiration.
- The cerebral cortex sends impulses to the respiratory center in response to strong emotions, such as anxiety, fear, and anger.
- Some sensory stimuli, such as irritating vapors may cause reflex inhibition of respiration.
- Disorders
- Emphysema
- Cystic Fibrosis
- Pneumonia
Ok got it. Now, are you ready for a recap? Here’s a lecture notes remix:
The Respiratory System-Remix
Introduction
Primary Function: obtaining oxygen and removing carbon dioxide
Other functions: Filter air, produce sounds, sense of smell, regulation of blood pH
Respiration: the process of gas exchange between the atmosphere and body cells
- Movement of air into the lungs – Ventilation
- Gas exchange between blood and air (external respiration)
- Gas transport in blood
- Gas exchange between the blood and body cells (internal respiration)
Cellular Respiration – the process of oxygen use and CO2 production at the cellular level
Organs of the Respiratory System
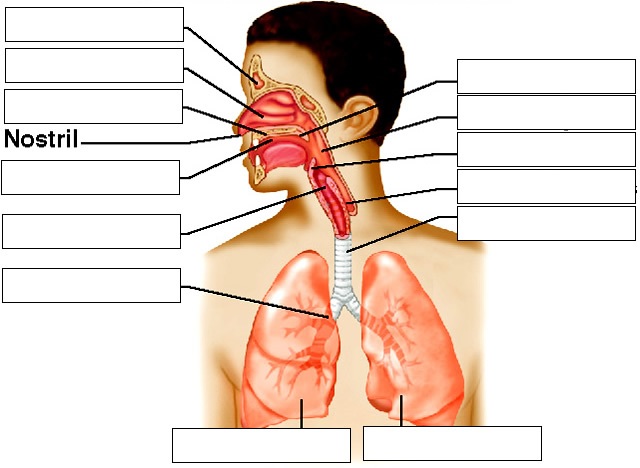
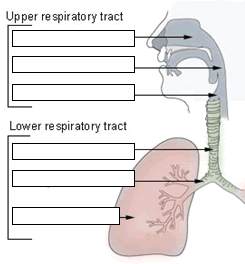
Upper Respiratory Tract – nose, nasal cavity, paranasal sinuses, pharynx
Lower Respiratory Tract – larynx, trachea, bronchial tree, lungs
Nose – bones and cartilage support nose, two openings (nostrils), hair filters large particles
Nasal Cavity – hollow space behind the nose | Nasal septum – divides the nose (bone)
Nasal conchae – bones that divide the nasal cavity, support the mucus membrane and increase surface area (superior, middle, inferior)
* deviated septum – when the septum bends to one side
— air is warmed as it enters the nasal cavity, sticky mucus traps particles which are pushed toward the pharynx and swallowed.
Paranasal Sinuses – spaces within the maxillary, frontal, ethmoid and sphenoid bones; reduce the weight of skull and are resonant chambers for voice.
Pharynx – behind the oral cavity, between the nasal cavity and larynx (space, not a structure) – nasopharynx, oropharynx, laryngopharynx
Larynx – enlargement at the top of the trachea and below pharynx, conducts air in and out of trachea, houses vocal cords
– composed of a framework of muscles and cartilages (thyroid (Adam’s apple), cricoids, epiglottic cartilages)
– false vocal folds (do not produce sound) – help close airway during swallowing
– true vocal folds (produce sound) – changing shape of the pharynx, and oral cavity changes sounds into words
– contracting and relaxing muscles changes pitch (increased tension = higher pitch)
Glottis – triangular slit that opens during breathing/talking, and closes during swallowing
Epiglottis – flaplike structure that stands upright, allows air to enter larynx, during swallowing it presses downward and prevents food from entering air passages
*Laryngitis – when the mucus membrane becomes swollen and prevents the vocal cords from vibrating freely
Trachea (windpipe) – flexible cylinder, about 12.5 cm long, extends downward in front of the esophagus
– contains about 20 C-shaped pieces of hyaline cartilage that prevent trachea from collapsing
Bronchial Tree – branched airways leading from the trachea to the air sacs in the lungs
Primary bronchii – left and right bronchioles alveolar ducts alveolar sacs alveoli
Gases are exchanged between alveoli and the blood stream
Lungs – soft spongy, cone-shaped organs in the thoracic cavity. The visceral pleura attaches to each lung surface and folds back to form the parietal pleura. The space between the visceral and parietal pleura is called the pleural cavity. Pleural cavity contains serous fluid to lubricate surfaces during breathing.
Left Lung – smaller, 2 lobes | Right Lung – larger than left, 3 lobes
16.3 Breathing Mechanism
Inspiration = inhalation | Expiration = exhalation
INHALATION
1. The diaphragm moves downward and the atmospheric pressure in the alveoli falls, which forces air into the airways
2. External intercostals muscles contract, raising ribs and sternum and enlarges the cavity even more
3. Pleural membranes held tightly together, move with the contractions of muscles
4. Surface tension in the alveoli (caused by water) makes it difficult to inflate them. Surfactant reduces tendency of alveoli to collapse. (Lack or surfactant in preemies can cause respiratory distress)
5. A deeper breath can be achieved through other muscles – pectoralis minor and sternocleidomastoid
6. The first breath of a newborn is the hardest because all of the alveoli are only partially inflated.
*Since our breathing is based on atmospheric pressure (and the difference in the pressure in the lungs), if there is a hole in the pleural cavity, the lung collapses (deflates). This can happen if a person is stabbed or a broken rib pierces the lung.
EXHALATION
1. As diaphragm and other muscles relax, elastic recoil from surface tension forces air out
2. If a person needs to exhale more air, internal (expiratory) intercostals muscles contract. Abdominal wall muscles (internal and external obliques, rectus abdominus and transverses abdominus) can help squeeze out more air.
3. These contractions increase the air pressure within the pleural cavity, forcing air out
NON-RESPIRATORY MOVEMENTS – Used to clear air passageways (coughing, sneezing) or express emotion (laughter, crying) – result from reflexes — A hiccup is a sudden inspiration due to a spasm of the diaphragm, air striking vocal folds makes the sound —A yawn may be caused by not enough blood becoming oxygenated, a yawn forces a deep breath
RESPIRATORY AIR VOLUMES AND CAPACITIES
Spirometry – measures volumes of air moving in and out of the lungs. 4 distinct respiratory volumes
Respiratory cycle – 1 inspiration + the following expiration1. Resting Tidal volume – amount of air that enters the lungs during 1 cycle
2. Inspiratory and 3. Expiratory reserve volume – after forced inhalation or exhalation
4. Residual Volume – air remaining in the lungs even after forceful exhalation
*** Combining two or more of the respiratory volumes = respiratory capacities.Inspiratory Reserve Volume + Expiratory Reserve Volume + Tidal Volume = Vital Capacity (maximum amount of air a person can exhale)
Tidal Volume + Inspiratory Reserve Volume = Inspiratory Capacity (max amount that can be inhaled)
Expiratory Reserve Volume + Residual Volume = Functional Residual Capacity (volume that remains in the lungs, resting)
Vital Capacity + Residual Volume = Total Lung Capacity (varies by sex, age, body size)
LABELING
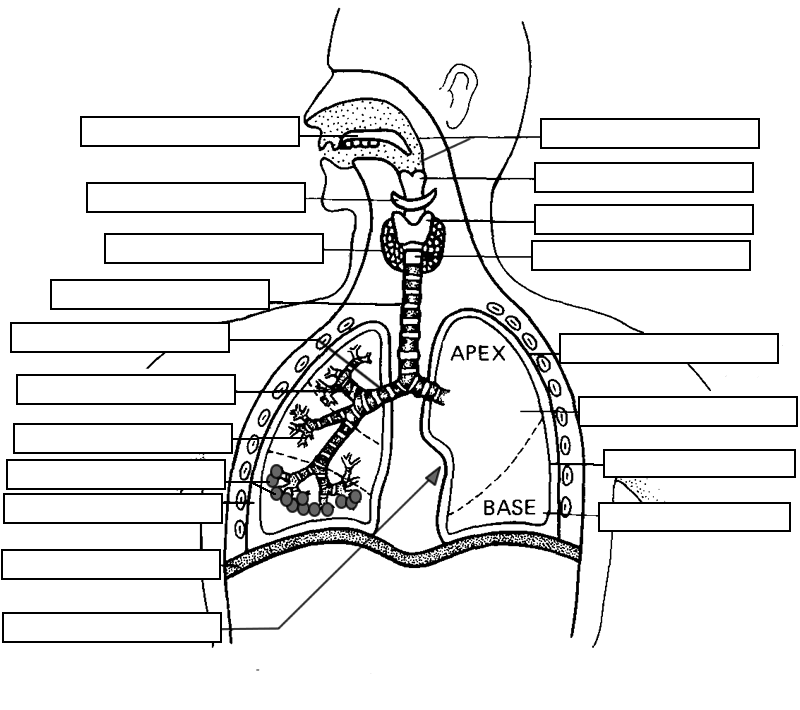
16.4 Control of Breathing
Breathing is an involuntary act, the muscles are under voluntary control (we can choose to hold our breath)
Respiratory Center – groups of neurons in the brain that control inspiration and expiration (based in the medulla and the pons)
Medulla Rhythmicity Area (Medulla) – two neuron groups extend the length of the medulla oblongata
Dorsal Respiratory Group – controls basic rhythm of respiration
Ventral Respiratory Group – generate impulses o increase respiratory movements, forceful expiration
Pneumotaxic Area (Pons) – inhibit respiratory bursts originating from the dorsal resp group
Factors Affecting Breathing
*Chemosensitive areas – detect concentrations of chemicals like carbon dioxide and hydrogen
1. Rise in CO2
2. Low blood oxygen (peripheral chemoreceptors, carotid and aortic bodies, sense changes)
3. Inflation reflex – regulates the depth of breathing, prevents overinflation of the lungs
4. Emotional upset, fear and pain
*hyperventilation – increase breathing for a short time lowers the blood CO2 concentration and will allow you to hold your breath for a longer period
The thin respiratory membrane allows other solutes (alcohol) to diffuse across it and be exhaled breath analysis
Alveolar Gas Exchanges
Alveoli – clusters or air sacs at the end of the bronchioles
Respiratory Membrane – layers of simple squamous cells and capillaries
Oxygen and CO2 exchange occurs by diffusion
Gas Transport
Oxygen combines with hemoglobin in the blood (oxyhemoglobin / deoxyhemoglobin)
Hypoxia – oxygen defiency. Can be caused by inadequate bood flow, poisons (cyanide and carbon monoxide)
Asphyxia – excess CO2 in the blood, lack of oxygen
ILLNESSES RELATED TO THE RESPIRATORY SYSTEM
1. Cystic Fibrosis (genetic)
2. Asthma
3. Bronchitis
4. Apnea
5. Emphysema
6. Lung Cancer
7. Altitude Sickness
8. Chronic Obstructive Pulmonary Disease (COPD)
9. Sinusitis
10. Bacterial or Viral Infections (cold, flu, pneumonia